Platelets are formed in the bone marrow where it undergoes a long production and maturation process under the influence of natural body minerals and other factors. However, the display of low platelet count in pregnancy can be possible due to alterations brought about by medical conditions. Some of which are discussed herein.
If a person develops low platelet count while pregnant, it can be associated to one of the following factors at play or probably all of the three: (1) Reduced production; (2) Increased destruction; and/or (3) Sequestration.
A very low level of platelet count can be dangerous especially with evident bleeding. It will certainly be a horrible situation to experience sudden and uncontrolled flow of blood from the nose, gums, or any other openings of the body.
And sadly, it could happen with a really low platelet count. Before that happens, early management must be performed immediately to prevent progression in the drop of levels.
It may usually be a costly endeavor but there are affordable options such as all-natural remedies you can learn from money back guaranteed materials like Conquer Low Platelets.
Low platelet count during pregnancy
Common conditions that can cause low blood platelets during pregnancy are as follows:
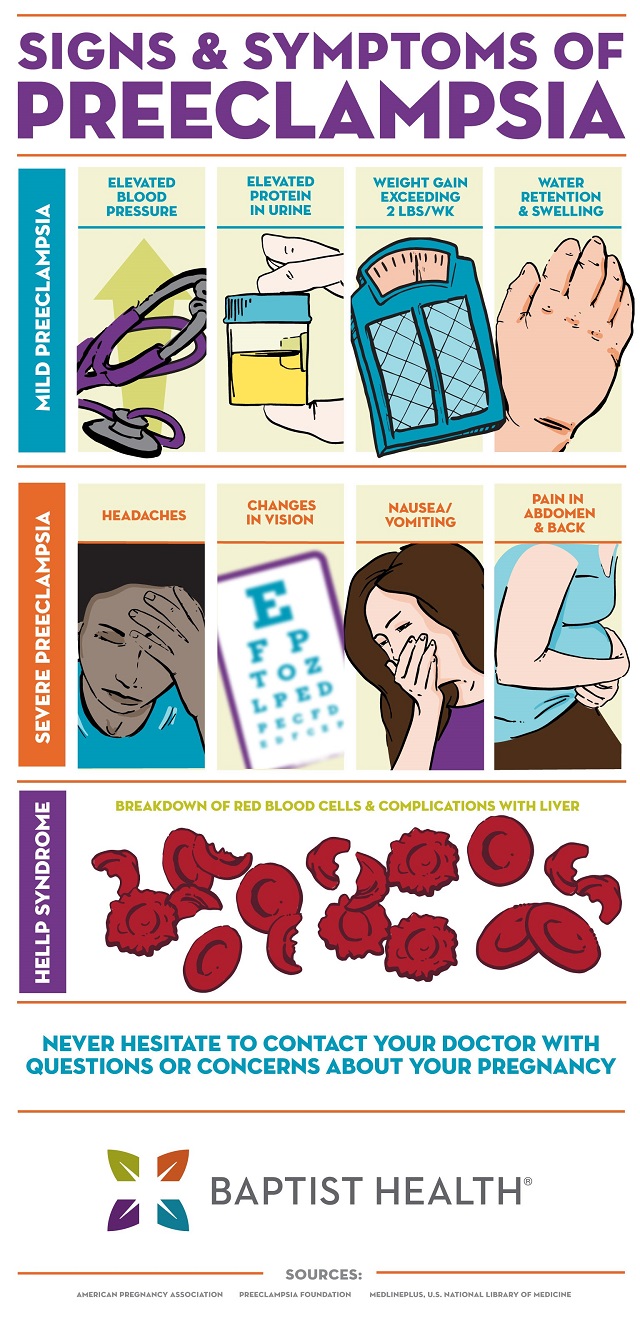
1. Preeclampsia or eclampsia.
Preeclampsia is a disorder exclusive to pregnant women where the blood pressure rises to abnormal levels. This increases the risk of damage to different organs of the body for both the mother and more significantly, the fetus.
Eclampsia is a severe form of the condition where the increase in blood pressure can result to damage that becomes apparent and accompanied by seizures.
It is a serious medical condition that warrants urgent management. Both conditions can be detected at an early stage following routine measurement of blood pressure levels in which every pregnant individual should undertake.
2. HELLP syndrome.
An advanced form of preeclampsia and eclampsia syndrome is HELLP syndrome. The elevation of blood pressure causes damage to the liver and increases the amount of liver enzymes in the blood.
A damaged liver means death of the cells that normally contain the enzymes. These cells, upon death, release these enzymes of the liver into the bloodstream.
It can be associated with low platelets due to the fact that liver function is required in the formation of platelets. The liver and kidneys also produce erythropoietin that stimulates the bone marrow to produce red blood cells. This hormone is found to have ample effects in regulating platelets.
HELLP means hemolysis of red blood cells, elevated liver enzymes and low platelets.
3. Heparin-induced thrombocytopenia.
It may be easy to say that no individual worldwide has never suffered from common colds. But when the illness is associated with streptococcus along with being improperly treated, it can lead to the development of valvular heart diseases. These diseases can make a person become vulnerable to the development of abnormal blood clots in the body.
There are several factors that can cause abnormal blood clotting in a person which can be damaging and life threatening. In order to prevent blood clots from harming the person, heparin use is usually suggested.
The use of heparin is a known and established rare causative factor associated to the development of thrombocytopenia in pregnancy. The development of low platelet count that results from the use of heparin is a condition referred to as Heparin-induced thrombocytopenia.
Considering that there are significant reasons where use of heparin is needed in pregnant woman, it puts them at risk to display a low platelet count.
When heparin is introduced into the body, it may cause the development of antibodies against the drug which influences an activation of platelets. It causes platelets to misbehave with adhesion and aggregation processes resulting to increased consumption that eventually leads to a low platelet count.
- Lindhoff-Last E, Bauersachs R (2002). Heparin-induced thrombocytopenia-alternative anticoagulation in pregnancy and lactation.
- M.Bardett Fausett, MD, M. Vogtlander, MD, R.M. Lee, MD, M.S. Esplin, MD, D.W. Branch, MD, G.M. Rodgers, MD, PhD, R.M. Silver, MD (2009). Heparin-induced thrombocytopenia is rare in pregnancy.
4. Immune Thrombocytopenic Purpura (ITP).
Immune thrombocytopenic purpura is an autoimmune hematologic disorder of manifesting reduced platelets in the body. It is mediated by immune cells and antibodies of the body that results in a destruction of platelets. It can be classified into two types – primary and secondary.
When the exact cause of immune destruction cannot be mediated it is termed as primary or idiopathic thrombocytopenic purpura.
When the cause of the immune destruction is mediated such as SLE or Hepatitis C, it is termed as secondary thrombocytopenic purpura.
5. Systemic Lupus Erythematosus (SLE).
Systemic lupus erythematosus is an autoimmune disease where the body attacks itself.
Pregnancy is one of the many conditions that can precipitate or aggravate SLE. In autoimmune diseases, antibodies are formed against the natural components of the body causing it to attack various organs, trying to destroy them.
One of commonly targeted organs is the bone marrow where platelets and other blood cells are born, developed, and matured. A destruction of the bone marrow results to a fall in the number of all types of blood cells released to the bloodstream.
6. Drug-induced.
There are many drugs that can alter any phase in the steps of platelet formation starting from the totipotent stem cell to megakaryocyte production.
Some of the drugs are known to be used during the period of pregnancy such as fluconazole which is an antifungal agent; ibuprofen and naproxen which are painkillers; and paracetamol which is a very common drug used for fever and headache.
No drug should be taken without prior discussion with a physician, especially in pregnant women for it won’t only affect a single person but two, including the fetus.
7. HIV/AIDS.
HIV is a sexually transmitted illness that started dominance in the beginning of this century. It can spread through blood and blood products, sexual contact, as well as from the parent to her child (when the child is in the mother’s womb).
HIV indirectly attacks all the systems of the body. This includes destroying the immune system of a person which is supposedly the only primary defense system to protect the body.
A weakened immune system gives opportunity to many type of infections that hover around the body for successful invasion. Some of these infections cause destruction of the bone marrow, which also means a destruction of platelets.
When HIV destroys the bone marrow, it can reduce the platelet count directly.
8. Aplastic anemia.
Aplastic anemia is a disease that also affects platelet levels because of an impaired bone marrow. The condition is possible during pregnancy, similarly causing a reduction in platelet count.
Aplastic anemia means the shutting or slowing down of bone marrow blood cell production. The cause of damage can be due to a bacteria, virus, drug, autoimmunity, or irradiation.
Depending on the cause of aplastic anemia in the pregnant woman, the treatment will vary.
9. Disseminated Intravascular Coagulation (DIC).
Disseminated intravascular coagulation is a disease that can be associated with a number of pregnancy-related medical conditions but can also be the pregnancy itself.
In DIC, there is widespread clotting that causes a consumption of platelets inside the blood vessels. This also results to a low platelet count.
Some conditions that can give rise to DIC during pregnancy is the presence of infection as well as autoimmune disorders.
10. Cancer.
There are different kinds of cancer that can affect a person depending on present predisposing risk factors. Pregnancy can be one of the risk factors for certain types.
Myelodysplastic syndromes and lymphoproliferative syndromes are common types of cancer that can affect pregnant women where low platelet count can be observed.
These medical conditions destroy the bone marrow and take up the space normally used for platelet formation and replacing it with cancer cell growth. They can also cause disseminated intravascular coagulation.
Low Platelet Count in Pregnancy is NOT Very Common
This is not a full exclusive list to detail causes of low platelet count in pregnancy but covers some of the common ones. Read essentials about normal platelet count in pregnancy.
Low platelet count in pregnancy is not a very common condition but can be present in a significant number of patients. It is found to be observed in nearly 5 to 8 percent of women in their pregnancy. The condition can be detected at an early stage with routine blood tests and follow up during the course of pregnancy. Therefore, regular check-up is essential.
The importance of regular follow-up cannot be emphasized enough.
- READ MORE